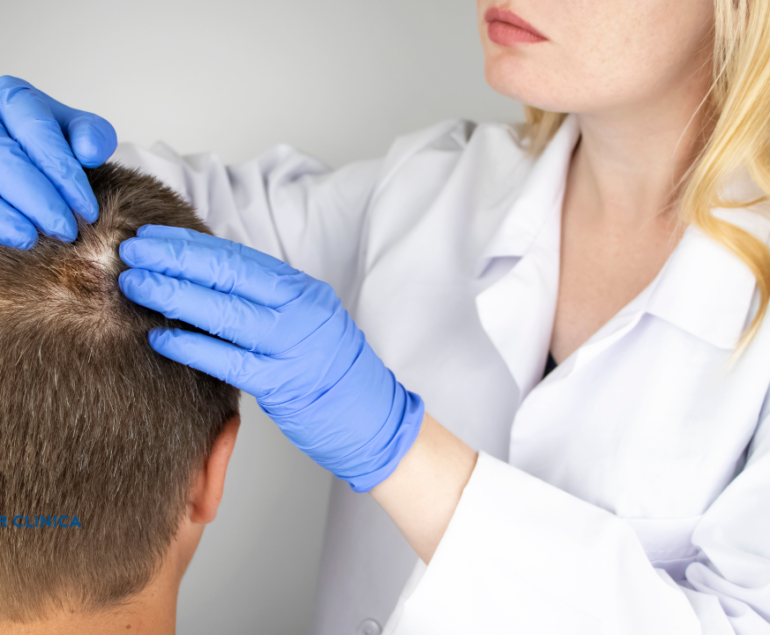
After a hair transplant, most people naturally focus on the transplanted area. Questions like “Will the grafts survive?”, “When will the scabs fall off?”, “When will my new hair start growing?” often come first. That is completely understandable.
However, there is another area that deserves just as much attention during recovery: the donor area.
The donor area is the region where hair follicles are taken from during hair transplant surgery. In most cases, this is the back of the scalp, especially the nape area. After the procedure, it is common to experience sensitivity, mild pain, itching, redness, small pimples, or scabbing in this region.
So, are these symptoms normal? When should you be concerned? Should pimples in the donor area be squeezed? What can be done if itching becomes uncomfortable? How long does donor area pain usually last?
In this guide, we will discuss pain, itching and pimple-like bumps in the donor area after hair transplant in a clear, realistic and patient-friendly way.
What Is the Donor Area in Hair Transplant?
The donor area is the region from which healthy hair follicles are collected during hair transplantation. In FUE hair transplant, hair follicles are usually extracted one by one from the back of the scalp.
During this extraction process, very small micro-openings are created in the skin. After the procedure, these tiny areas begin to heal. This healing phase may involve tenderness, mild pain, tightness, scabbing, itching or redness.
In many cases, these signs are part of the normal tissue repair process. However, not every symptom should automatically be considered normal. The severity, duration and progression of the symptom matter.
A mild discomfort that gradually decreases is usually different from pain that becomes worse day by day. This is why patients should follow the post-operative instructions given by their medical team and report unusual symptoms.
Why Does the Donor Area Become Sensitive After Hair Transplant?
During hair follicle extraction, the skin in the donor area experiences controlled micro-trauma. This does not mean something has gone wrong. It simply means that the skin has gone through a medical procedure and now needs time to repair itself.
The body responds by increasing blood flow, starting tissue repair and closing the tiny extraction points. During this process, patients may feel tightness, burning, tenderness, stinging or mild pain.
You can think of it like a small skin scratch healing. As the skin repairs itself, it may form scabs and become itchy. The donor area goes through a similar healing process, but on a larger and more organized scale.
The key point is this: symptoms should generally improve over time. If pain, redness, swelling or discharge increases instead of decreasing, the area should be evaluated by a healthcare professional.
Is Pain in the Donor Area Normal After Hair Transplant?
Mild to moderate pain in the donor area may be expected after hair transplant. Especially in the first few days, the back of the scalp may feel sensitive, tight or sore.
This discomfort is usually related to the healing of the micro-extraction points. The number of grafts taken, the duration of the procedure, the person’s skin structure, pain threshold and extraction technique can all influence the level of discomfort.
Some patients describe it as “just a mild sensitivity,” while others may feel more noticeable soreness during the first days. This difference is normal because every person heals differently.
How Long Does Donor Area Pain Last?
In many patients, donor area pain begins to decrease within the first few days. Noticeable relief is often expected within the first week. However, some people may continue to feel tightness, numbness or sensitivity when touching the area for a longer period.
The character of the pain is important. Pain that is mild, manageable and gradually improving is generally part of the expected recovery process. However, pain that becomes stronger, throbbing, hot, swollen or associated with discharge should not be ignored.
If the pain feels unusual or is getting worse, the safest approach is to contact the medical team that performed the procedure.
What Can Help Reduce Donor Area Pain?
The most important rule is to follow your physician’s instructions. Patients should not use random medications, creams or home remedies without medical approval.
In general, the following points may help protect the donor area during recovery:
Avoid pressure on the donor area. In the first days, friction from pillows, tight collars, hats or hard surfaces can increase sensitivity.
Pay attention to sleeping position. Your physician may recommend sleeping with your head elevated or supported in a certain way to protect both the transplanted area and the donor area.
Use pain relief only if recommended. Some painkillers may affect bleeding or bruising risk, so medication should be used according to medical advice.
Do not rub, scratch or aggressively wash the area. The skin is already healing, and unnecessary trauma may increase irritation.
Why Does the Donor Area Itch After Hair Transplant?
Itching is one of the most common complaints after hair transplant. In fact, some patients say itching is more annoying than pain. This is understandable because itching can be persistent and uncomfortable.
There are several possible reasons for itching in the donor area. One of the most common causes is skin healing. As the tiny extraction points close, scabs form and the skin renews itself, itching may occur.
Dryness can also contribute to itching. After hair transplant, special shampoos, cleansing routines, antiseptic products or temporary changes in the skin barrier may cause dryness. Dry skin tends to itch more.
Scabbing may also increase the urge to scratch. Scabs are part of the natural healing process, but picking or scratching them can irritate the skin and increase the risk of infection.
Is Donor Area Itching Normal?
Mild itching can be considered normal during the early recovery period. It is especially common during the scabbing and healing stages.
However, the intensity of itching matters. Mild and tolerable itching is usually part of recovery. Severe itching, spreading redness, blisters, discharge or rash-like reactions should be discussed with a physician.
Sometimes itching may be related to an allergic reaction or irritation caused by a product. For this reason, it is not always correct to say, “It is normal, it will pass,” without evaluating the whole picture.
What Can Help Reduce Itching?
The most important step is not to scratch the donor area. I know this is easier said than done. When an area itches, the natural instinct is to scratch it. But scratching with nails may damage the skin, remove scabs too early and increase irritation.
Follow the washing routine recommended by your clinic. If you were given a special shampoo, lotion or post-care protocol, use it exactly as instructed.
Avoid harsh or unknown products. Alcohol-based products, perfumes, random antiseptics, cosmetic oils or homemade mixtures may irritate the skin further.
Keep the scalp clean but do not over-clean. Excessive washing or harsh rubbing can dry the skin and make itching worse.
If itching becomes very uncomfortable, speak with your medical team. Your physician may recommend a suitable moisturizing approach, medication or adjustment in your care routine if necessary.
Why Do Pimples Appear in the Donor Area After Hair Transplant?
Small pimple-like bumps may appear in the donor area after hair transplant. This can worry patients because they may wonder, “Is this an infection?”
There are several reasons why pimple-like bumps may occur. Sometimes they are related to the healing process of the skin and hair follicles. Oil balance, scabbing, temporary irritation and post-operative care products may all play a role.
In some cases, folliculitis may develop. Folliculitis is inflammation of the hair follicle and may appear as small red, tender or pus-filled bumps. Mild cases may improve with proper care, while some cases may require medical treatment.
Are Pimples in the Donor Area Normal?
Small, limited and mild pimple-like bumps may be seen during the recovery period. However, if pimples increase in number, become painful, look inflamed, produce discharge or are accompanied by warmth and redness, the area should be evaluated.
If pimples are associated with worsening pain, bad smell, spreading redness, fever or general weakness, medical advice should be sought without delay.
A simple way to think about recovery is this: normal healing usually improves gradually. Infection or significant inflammation often gets worse instead of better.
Should Pimples in the Donor Area Be Popped?
No. Pimples or pimple-like bumps in the donor area should not be squeezed or popped.
Squeezing them may cause irritation, bleeding, infection spread or increased risk of scarring. The donor area is already sensitive after the procedure, so any unnecessary trauma can make recovery more difficult.
If the bumps become painful, inflamed or widespread, consult your physician. The medical team may recommend proper cleansing, topical treatment or another medical approach if needed.
How Should the Donor Area Be Cared For?
The safest donor area care is the one recommended by the medical team that performed your hair transplant. Each clinic may have its own washing routine, dressing protocol and product recommendations depending on the technique used.
Still, the general logic is similar: keep the area clean, avoid irritation, do not scratch, do not pick scabs and do not apply random products.
Donor Area Care in the First Days
In the first few days, the donor area may be sensitive. During this period, avoid direct pressure on the back of the scalp. Friction from pillows, collars, hats or rough contact may increase discomfort.
The timing of the first wash should be determined by your clinic. In some cases, the first wash is performed at the clinic. In others, the patient is given detailed instructions for washing at home.
Many patients think, “If I clean it more, it will heal faster.” But excessive intervention is not always helpful. Gentle care is often the foundation of healthy recovery.
What Should Be Considered During Washing?
When washing the donor area, avoid strong water pressure. Do not use nails. Do not rub the area aggressively. Do not try to remove scabs by force.
If your physician recommended a shampoo or lotion, apply it as instructed. Random products may dry or irritate the scalp.
After washing, do not rub the area harshly with a towel. The donor area should be dried gently or left to dry according to your clinic’s recommendations.
Care During the Scabbing Period
Scabbing is a natural part of healing after hair transplant. Small scabs may also form in the donor area. These scabs should not be picked, scratched or forcibly removed.
With proper washing and care, scabs usually soften and fall off over time. Patience is important here. Trying to remove scabs too early may irritate the skin.
If the scabs are causing intense itching, the best step is not to scratch them, but to contact your clinic and ask whether your care routine needs adjustment.
Is Numbness or Tingling in the Donor Area Normal?
Numbness, tingling or a stinging sensation may occur in the donor area after hair transplant. This may be related to temporary irritation of small nerve endings in the skin.
In many patients, these sensations gradually decrease. However, the recovery period varies from person to person. Some people feel better within a few weeks, while others may experience mild sensitivity for a longer time.
If numbness becomes worse, turns into severe pain or feels like intense electric shocks, it should be discussed with a physician. Not every symptom should be assumed to be part of normal recovery.
When Does Redness in the Donor Area Go Away?
Redness in the donor area may be expected after hair transplant. It may be more visible in people with fair or sensitive skin.
In general, redness should gradually decrease over time. Redness that is obvious in the first days should become lighter as healing progresses.
However, spreading redness, increasing warmth, pain, swelling or discharge should not be considered routine healing. These signs may require medical evaluation.
The direction of change is important. Redness that is improving is usually less concerning. Redness that is spreading or worsening should be checked.
What Are the Signs of Infection in the Donor Area?
Infection after hair transplant is not common, but it is important to recognize warning signs early. Early communication with the medical team can help manage possible problems more effectively.
You should contact your physician if you notice:
Pain that increases instead of decreasing
Spreading redness in the donor area
Warmth, swelling and tenderness
Pus-like discharge or bad smell
Fever or general weakness
Rapidly increasing pimple-like lesions
Severe pain or discharge under scabs
Persistent bleeding
If these symptoms occur, do not use random creams, antibiotics or herbal mixtures at home. Treatment should be planned after medical evaluation.
Are Pimples and Folliculitis the Same Thing?
Not every pimple is folliculitis, but some pimple-like bumps after hair transplant may be related to folliculitis. Folliculitis refers to inflammation or infection around the hair follicle.
Small, isolated and painless bumps may simply be related to healing. However, red, tender, pus-filled or painful bumps should be evaluated.
The correct distinction should be made by a physician. From the outside, scabs, pimples, ingrown hairs and inflamed lesions may look similar.
What Can Be Done at Home for Donor Area Pimples?
The safest thing to do at home is to keep the area clean and calm. Do not squeeze pimples. Do not pick scabs. Do not apply alcohol, cologne, random antibiotic creams or herbal products.
Continue the washing routine recommended by your clinic. If your products cause excessive dryness, burning or more itching, inform your medical team.
If the bumps are mild and not spreading, they may only need observation. But if there is pain, discharge, increasing redness or spreading lesions, medical evaluation is necessary.
Why Is Scratching the Donor Area Risky?
Scratching may feel relieving for a few seconds, but it can cause problems in the longer term. Nails can scratch the skin surface, remove scabs too early and introduce bacteria to the healing area.
During the first weeks, the donor area is still recovering. Mechanical trauma can increase irritation and delay comfort.
If itching becomes difficult to tolerate, do not try to solve it by scratching. Contact your clinic. Your physician can evaluate whether itching is related to dryness, healing, allergy or infection.
Daily Habits That May Support Donor Area Recovery
Recovery is not only about external products. Sleep, hydration, nutrition, hygiene and lifestyle habits can also affect the healing process.
Sleeping Position
In the early period, sleep in the position recommended by your physician. Protecting the scalp from friction and pressure can help reduce discomfort.
Using a clean pillowcase is also important. Sweat, oil and dirt may irritate the healing skin.
Controlling Sweating
Heavy exercise, sauna, steam rooms or hot environments may increase sweating during the early recovery period. Sweat may trigger itching or irritation on sensitive skin.
Avoid intense activity until your physician allows it. This is not about being overly cautious; it is about giving the skin time to heal calmly.
Nutrition and Hydration
Balanced nutrition supports tissue repair. Adequate protein, vitamins and minerals may contribute to the body’s healing capacity.
Hydration is also valuable for skin health. Drinking water alone will not solve pimples or itching, but it supports general recovery.
Smoking and Alcohol
Smoking may negatively affect blood circulation. Alcohol may contribute to swelling, bleeding risk or delayed recovery in some individuals.
Your medical team may recommend avoiding smoking and alcohol for a certain period after hair transplant. It is best to follow the instructions given specifically for your case.
What Should Not Be Done to the Donor Area?
Sometimes patients try to speed up healing and unintentionally irritate the skin. The following should generally be avoided unless your physician says otherwise:
Do not scratch the donor area with your nails.
Do not squeeze or pop pimple-like bumps.
Do not pick or forcefully remove scabs.
Do not apply random creams, oils, lotions or herbal mixtures.
Do not massage the area aggressively.
Do not wash with very hot water.
Do not wear tight hats or clothing that rubs against the donor area.
Do not use medications outside your physician’s recommendations.
These may sound like small details, but after hair transplant, small mistakes may create unnecessary discomfort.
Why Does the Donor Area Cause Anxiety After Hair Transplant?
After hair transplant, many patients check the mirror frequently, take photos and compare their progress day by day. This is very common. Hair transplant is not only a physical process; it is also emotionally important for many people.
A few pimples in the donor area can make someone worry: “Is my scalp healing incorrectly?”, “Will there be a scar?”, “Did something go wrong?”
The healthiest approach is neither panic nor complete neglect. Mild pain, itching, scabbing and limited bumps may be part of recovery. But symptoms that worsen should be taken seriously.
Balanced observation is the key. Watch the healing process, follow instructions and communicate with your clinic when something feels unusual.
Donor Area Care and Health Tourism in Istanbul, Turkey
Forever Clinica is a health tourism agency in Turkey that may support international patients with planning, communication and coordination during their hair transplant journey. For patients traveling to Istanbul, Turkey, post-operative care is especially important because many questions may arise after the procedure.
Pain, itching, pimples, redness and scabbing in the donor area should be explained clearly to patients. They should know which symptoms may be part of expected healing and which symptoms require medical contact.
A good hair transplant experience is not limited to the operation day. Post-operative care, follow-up, proper communication and realistic expectations are also essential parts of the process.
For international patients, organization support such as appointment planning, translation, accommodation, transfer coordination and post-procedure guidance can make the journey easier to understand. However, all medical decisions and treatment recommendations should be made by authorized healthcare professionals.
When Should Donor Area Symptoms Be Taken Seriously?
You should contact your physician if:
Pain gets worse day by day
Itching becomes unbearable
Pimple-like bumps spread quickly
There is pus or discharge
Redness spreads
The area becomes hot and swollen
Fever or weakness occurs
There is a bad smell
Bleeding continues
Numbness becomes worse or turns into severe pain
These symptoms do not always mean there is a serious problem, but they should be evaluated. Early communication can help prevent small issues from becoming bigger concerns.
When Does the Donor Area Feel Comfortable Again?
The recovery timeline varies from person to person. Pain and sensitivity may be more noticeable in the first few days. Many patients begin to feel more comfortable within the first week.
Scabbing and itching may appear at different stages of healing. Some patients recover quickly, while others may experience mild redness, tightness, numbness or sensitivity for a longer period.
The overall trend matters. If symptoms are decreasing and the skin looks calmer, recovery is usually moving in the expected direction. If symptoms increase or new problems appear, a check-up is recommended.
Conclusion: Donor Area Care Is a Quiet but Important Part of Hair Transplant Recovery
Pain, itching and pimple-like bumps in the donor area after hair transplant are common concerns. Mild pain, scabbing, itching and limited sensitivity may be part of the healing process. However, these symptoms should be monitored carefully.
Do not scratch the donor area. Do not squeeze pimples. Do not pick scabs. Follow your clinic’s washing and care instructions. If something seems unusual, contact your medical team instead of trying random solutions at home.
Hair transplant recovery is not only about the transplanted area. The donor area also needs time, care and protection. A calm recovery process depends on patience, proper hygiene and clear communication with healthcare professionals.
For patients considering hair transplant in Istanbul, Turkey, understanding the donor area recovery process before the procedure can make the experience more comfortable and realistic.
Frequently Asked Questions
Is pain in the donor area normal after hair transplant?
Yes, mild or moderate pain and sensitivity in the donor area may occur after hair transplant. This is usually related to the healing of the tiny extraction points. However, worsening pain should be discussed with a physician.
How long does donor area pain last?
In many patients, pain begins to decrease within the first few days and noticeable relief may occur within the first week. The duration may vary depending on skin structure, procedure intensity and personal healing response.
Why does the donor area itch after hair transplant?
Itching may occur due to skin healing, scabbing, dryness or sensitivity to care products. Mild itching can be expected, but severe or spreading itching should be evaluated.
What should I do if the donor area itches?
Do not scratch the area with your nails. Continue the washing and care routine recommended by your clinic. If itching is severe, contact your medical team.
Is it normal to have pimples in the donor area?
Small and limited pimple-like bumps may appear during recovery. However, painful, inflamed, spreading or pus-filled bumps should be checked by a physician.
Should donor area pimples be popped?
No. Pimples or bumps in the donor area should not be squeezed or popped. This may increase irritation, infection risk and scarring risk.
When does redness in the donor area go away?
Redness usually decreases gradually over time. It may be more visible in fair or sensitive skin. Spreading redness, warmth, pain or discharge should be evaluated.
Is numbness in the donor area normal?
Temporary numbness, tingling or stinging may occur after hair transplant. It often improves over time. Severe or worsening numbness should be discussed with a physician.
How should the donor area be washed?
The donor area should be washed gently according to the clinic’s instructions. Avoid strong water pressure, scratching with nails and forcefully removing scabs.
Can I apply cream to the donor area?
Do not apply random creams, oils, lotions or herbal products unless recommended by your physician. Incorrect products may irritate the skin.
How can I recognize infection in the donor area?
Increasing pain, spreading redness, warmth, swelling, pus-like discharge, bad smell, fever or general weakness may require medical evaluation.
When does the donor area fully heal?
Initial healing usually begins within days, but full skin calming varies from person to person. Mild redness, sensitivity or numbness may last longer in some patients.
Should scabs in the donor area be removed?
No. Scabs should not be picked or removed forcefully. They usually soften and fall off gradually with proper washing and care.
Can a hat irritate the donor area?
Yes, tight or rough hats may irritate the donor area in the early period. Follow your physician’s guidance on when and how to wear a hat.
What is the most important rule for donor area care?
Keep the area clean, avoid scratching, do not squeeze pimples, do not pick scabs and follow your physician’s post-operative instructions.